|
Additionally, we can and should work with radiologists to define evaluation criteria and improve what’s captured by radiography on the first try. “All physicians should be sure that the radiology facilities they refer patients to for spinal radiography employ every technology and safety measure available to limit radiation exposure. 
“Orthopaedic surgeons and pediatricians share the responsibility to ensure children are exposed to as little iatrogenic radiation as possible,” Dr. Study authors also reinforced the need to do everything possible to reduce radiation exposure for children through proper use of protective shielding for reproductive organs and digital radiograph technology. A full-length lateral view of the spine.The iliac crest as an indicator of skeletal maturity.A full coronal view of the spine including skull base and pelvis.Radiographic images that allow for proper evaluation of idiopathic scoliosis and reduce radiation exposure include: However, a few basic criteria could greatly reduce the number of repeat images necessary. Oetgen and the study authors note that there is currently no standardized protocol for spinal radiography of suspected idiopathic scoliosis. “It’s frustrating because in many cases, a simple change in how the initial radiograph was taken could have prevented the need for more imaging studies.”ĭr. “Repeating the radiograph means these kids received another exposure to radiation, too,” says Matthew Oetgen, M.D., the study’s lead author and chief of Orthopaedic Surgery and Sports Medicine at Children’s National Health System. If a child arrives at the pediatric orthopaedic specialist for an idiopathic scoliosis evaluation without an adequate radiographic image of his or her spine, it’s often necessary to order yet another imaging study for accurate assessment.Ī study published in the Journal of the American Academy of Orthopaedic Surgeons found that in a 6 month period, almost half (43 percent) of patients referred for evaluation required a repeat radiograph due to missing or poor quality existing images. Thus, in the present work, we discuss normal radiological features of the pediatric cervical spine, variants that may be encountered and pitfalls that must be avoided when interpreting plain radiographs taken in an emergency setting following trauma.Īnatomy Pediatric spine Radiograph Variants.Chief of Orthopaedics and Sports Medicine Matthew Oetgen, M.D., discusses an image of a patient’s spine. With it, the physician can, on one hand, differentiate normal physes or synchondroses from pathological fractures or ligamentous disruptions and, on the other, identify any possible congenital anomalies that may also be mistaken for injury. Comprehensive knowledge of the specific anatomy and biomechanics of the childhood spine is essential for the diagnosis of suspected cervical spine injury. The interpretation of a plain radiograph of the pediatric cervical spine following trauma must take into account the age of the child, the location of the injury and the mechanism of trauma. Such features as hypermobility between C2 and C3, pseudospread of the atlas on the axis, pseudosubluxation, the absence of lordosis, anterior wedging of vertebral bodies, pseudowidening of prevertebral soft tissue and incomplete ossification of synchondrosis can be mistaken for traumatic injuries. In all cases, the pediatric cervical spine has distinct radiographic features, making the emergency radiological analysis of it difficult. Young children aged less than 8 years usually have upper cervical injuries because of the anatomic and biomechanical properties of their immature spine, whereas older children, whose biomechanics more closely resemble those of adults, are prone to lower cervical injuries. The distribution of injuries, when they do occur, differs according to age. dangerous mechanism of injury (fall from a height of greater than 1 metre or 5 steps, axial load.  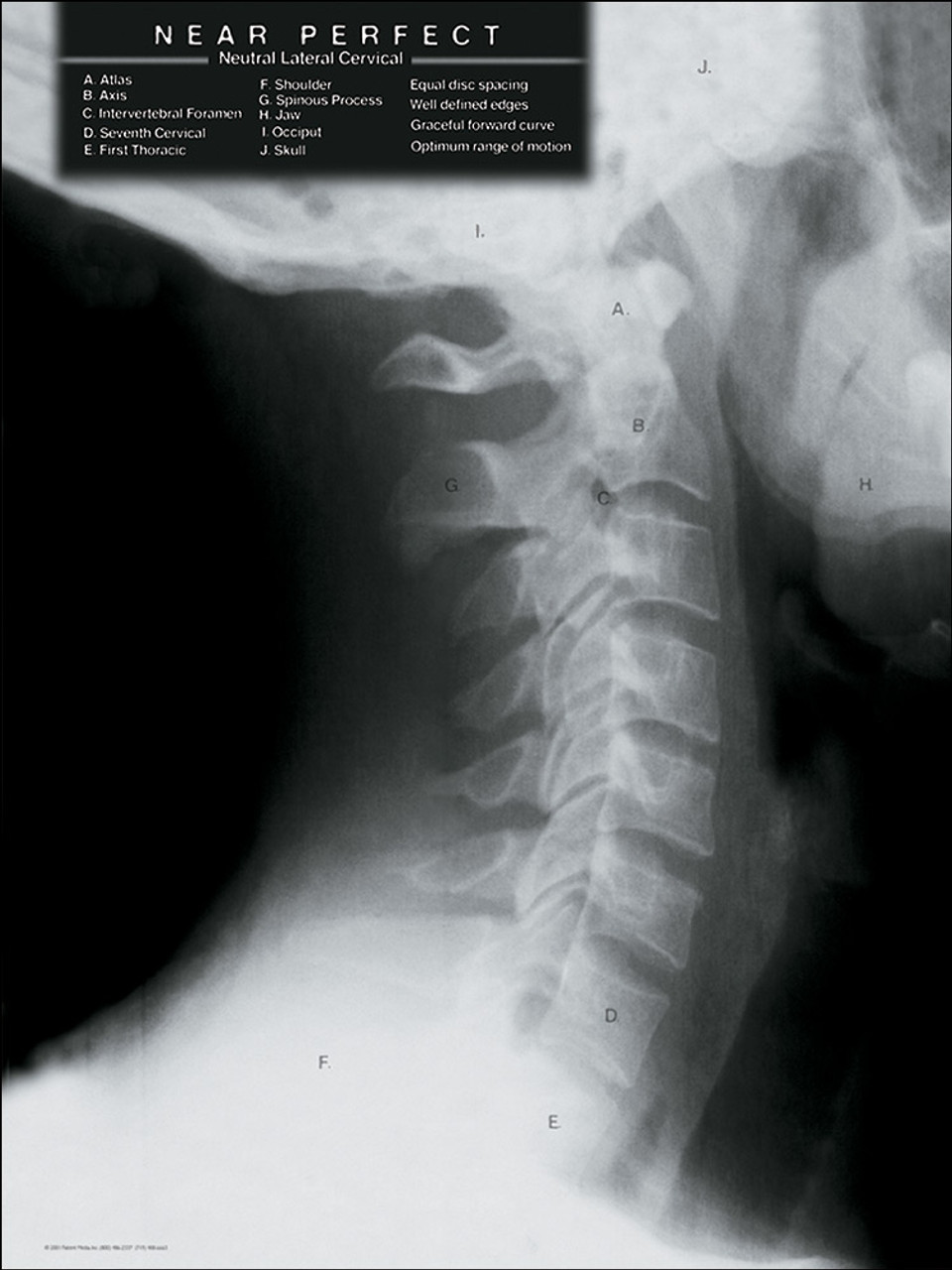
Injuries of the cervical spine are uncommon in children. The person with suspected spine injury should be assessed as having high, low or no risk of cervical spine injury using the following rule: the person is at high risk if they have at least 1 of the following high-risk factors: age 65 years or older.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
